Dementia is an umbrella term for various conditions that cause a progressive decline in mental function affecting memory, thinking, behavior, and reasoning, which significantly impacts a person’s ability to perform daily activities.
The causes are numerous and include Alzheimer disease, vascular dementia that can occur after a stroke, alcohol related causes, genetic and psychiatric disease, and traumatic brain injury. Globally, dementia is the seventh leading cause of death and a significant cause of disability and dependency in older adults. This results in a substantial financial burden on the healthcare sector and families, due to the cost of care and the loss of income for caregivers. Patients with dementia are more likely to be hospitalized, have a greater likelihood of experiencing functional decline, and experience other adverse outcomes during a hospital stay.
Dementia disproportionately affects women of color and is influenced by a mix of genetic, environmental, and socioeconomic factors. Globally, and in the Caribbean, dementia is projected to increase significantly in the coming decades, with women expected to continue to bear a disproportionate share of the disease, in part due to longer life expectancy and increased rates of chronic diseases. Many cases remain undiagnosed due to cultural beliefs that cognitive decline is a natural part of aging. While dementia risk increases after age 65, it is not a natural part of aging.

Older adults may experience slower processing speeds and occasional memory lapses, as well as a tendency to misplace items such as keys. These do not significantly disrupt daily activities. Dementia, however, leads to substantial cognitive decline, including the inability to recognize familiar objects and people, which affects basic tasks and daily functioning. One of the earliest signs is difficulty with instrumental activities of daily living (IADLs), which require higher-level cognitive skills, such as managing finances, transportation, shopping, meal preparation, and adhering to medication regimens. Missing appointments or struggling with bill payments often precede more noticeable impairment. Estrogen levels decline significantly during menopause, resulting in an increased risk of developing dementia and depression. Estrogen protects the brain through various mechanisms, including reducing inflammation and promoting neuronal growth and connectivity.
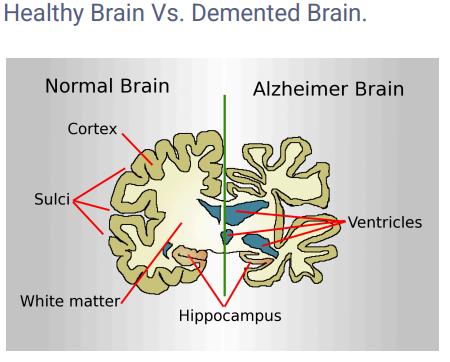
Alzheimer’s disease [AD] is the most common type of dementia worldwide. It is named after Dr. Alois Alzheimer, who described it in 1906. It is characterized by the buildup of abnormal proteins in the brain that damage brain cells and disrupt communication.
Vascular dementia is the second most common cause; a single stroke or multiple small strokes can damage brain tissue and lead to vascular dementia. Caused by treatable factors, such as smoking, hypertension, diabetes, and cholesterol. The increasing prevalence of smoking and alcohol consumption among Caribbean women is a growing concern. Smoking accelerates brain damage, raising the likelihood of vascular dementia. Alcohol consumption is deeply ingrained in Caribbean cultural celebrations, music, and sports. However, excessive alcohol intake is neurotoxic, leading to brain cell death and an increased risk of dementia. Don’t drink and drive; more than two is too many.
Risk factors for dementia are both non-modifiable or things we cannot control, such as age, where there is an increased incidence after the age of 65, family history of dementia, which increases risk, race, and genetic factors, including a higher occurrence of the APOE-e4 gene among African-descendant populations. This gene variant is a significant genetic risk factor for Alzheimer’s disease due to increased amyloid-beta plaque deposition in the brain.
Modifiable risk factors are things we can control. Managing conditions like hypertension, cholesterol, obesity, and diabetes through medication adherence and lifestyle adjustments with smoking and alcohol abstinence, healthy eating, and exercise can significantly reduce the risk of strokes, which in turn lowers dementia risk. Up to 40 % of dementia can be prevented by addressing social and underlying medical conditions.
Head injuries, including concussions and mild traumatic brain injury, increase the risk of dementia, particularly AD. After a concussion, “brain rest” or cognitive rest is crucial for brain healing.
The region is undergoing a significant lifestyle shift, moving away from traditional diets and active living toward Western-style fast food and sedentary habits, contributing to obesity, cardiovascular disease, and cognitive decline. Loneliness and social isolation have profound effects on mental health, especially among older Caribbean women. As they outlive their spouses and see their adult children migrate, they face emotional distress that can accelerate cognitive decline. Social isolation isn’t just about lacking companionship—sensory impairments compound it. Hearing and vision loss disrupt daily interactions, making communication, independent living, and engagement in routine activities more difficult and increasing dementia risk. Acetylcholine is the key neurotransmitter involved in memory and cognitive function; the level declines in Alzheimer’s disease, impairing new memory formation. Certain medications can exacerbate this depletion, increasing the risk of dementia. Drugs like older antihistamines, such as Benadryl, and benzodiazepines used for sleep and anxiety, like Valium and Xanax, should be avoided.
The Beers Criteria, available online, provides a comprehensive list of safer medication options for older adults. Current medical guidelines don’t support routine dementia screening for asymptomatic individuals. Families and caregivers often notice early signs, particularly after the loss of a spouse, which can remove a critical source of emotional and cognitive support. The resulting social isolation and decreased mental stimulation may accelerate cognitive decline.
Determining the specific type of dementia is crucial for accurate diagnosis and treatment. Since currently approved medications primarily target Alzheimer’s disease (AD), distinguishing between different forms is essential for effective management. General practitioners play a pivotal role in early assessment and management. Assessment is individualized but will include a clinical history, neurologic examination, cognitive assessments, brain imaging, and laboratory tests to rule out reversible causes, such as hypothyroidism, vitamin D, B12, and folate deficiencies. Medication reviews and depression screening are essential. Identifying high-risk medications that contribute to cognitive decline is crucial, as polypharmacy, particularly in older adults, can exacerbate symptoms. Depression and cognitive impairment frequently overlap. When cognitive difficulties stem from depression, appropriate treatment can lead to notable improvement, reinforcing the need for integrated mental health care in dementia evaluations. While blood tests for AD are advancing, they are expensive and not readily available. Several office-based screening tools are available for cognitive assessment, with the Mini-Cog being a quick and easy option. It combines a three-item recall test with a clock-drawing task, making it a practical tool for use in primary care settings. Other useful screening tools include the Montreal Cognitive Assessment (MoCA), which is valuable for assessing early cognitive impairment but may require more time to administer. A more detailed assessment uses the Mini-Mental State Examination (MMSE), which helps indicate the severity of cognitive impairment and estimate dementia severity based on the score.
Preventative Strategies
Dementia is closely linked to mental and cardiovascular health, social isolation, and depression, emphasizing the need for a comprehensive approach. It develops gradually, often rooted in unhealthy lifestyle choices such as poor diet, lack of exercise, smoking, and excessive alcohol consumption, which contribute to brain damage in midlife.
Prevention becomes essential and highly effective in resource-limited settings, such as those in the Caribbean. Approved medications are only for Alzheimer’s dementia and offer only modest benefits, primarily in mild to moderate cases. Early recognition of mild Alzheimer’s opens the door to multiple therapeutic options, while advanced disease shifts the focus to managing sleep disturbances, behavioral challenges, and ensuring comfort through palliative care. Additionally, lifestyle factors are crucial: brain stimulation through learning new tasks and hobbies, meditation, regular exercise, sunlight exposure, and social engagement, as well as avoiding air pollution, all play a role in supporting cognitive health. Routine dental, vision, and hearing screenings, adherence to medications for chronic conditions, and eliminating smoking and excessive alcohol consumption further strengthen long-term brain function. A heart-healthy diet featuring locally sourced produce, such as avocados, greens, and fish, is key to reducing inflammation and slowing cognitive decline. It also contributes to overall cardiovascular health and is vital for preventing dementia.
Support groups and family discussions help increase awareness and understanding. They encourage early discussions about living wills and end-of-life choices, as well as selecting a healthcare and financial proxy. Family support is essential to monitor for abuse; unscrupulous individuals frequently target the elderly to inflict financial abuse and identity theft. Demented patients are especially vulnerable to physical, emotional and financial abuse due to their dependency on others and impaired short-term memory. Palliative care offers numerous benefits to patients and their families, ensuring compassionate support, home-based care when feasible, reduced hospitalizations, and helping families navigate difficult decisions, anticipating challenges to reduce frustration and anxiety, fostering dignity and empowerment in medical decision-making.
This article provides a general overview of public education. Please consult your primary healthcare provider for an individualized evaluation if you have concerns about your brain health.